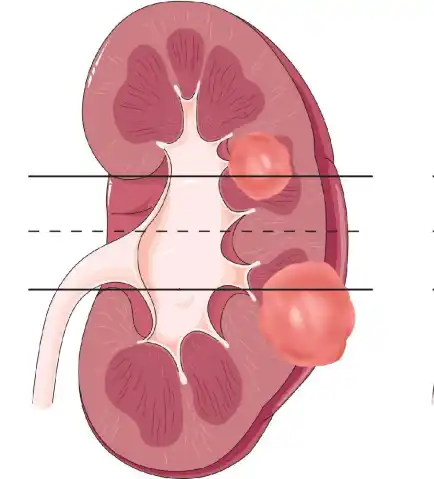
Bosniak Calculator for Renal Cystic Masses
More about the Bosniak Calculator for Renal Cyst Classification 2019
The Bosniak classification 2019 provides a standardized framework for cystic renal mass evaluation on CT and MRI, with the goal of improving consistency in lesion description, category assignment, and management discussions. In clinical practice, a Bosniak renal cyst calculator may help organize imaging features, but classification still depends on careful radiologist assessment of enhancement, wall and septal morphology, nodularity, and lesion composition.[1][3]
Evolution of the Bosniak system for complex renal cyst imaging
The original Bosniak system was developed for contrast-enhanced CT and became widely used for stratifying cystic renal lesions. The 2019 revision formally incorporated MRI, defined previously ambiguous morphologic terms, and shifted the system toward greater specificity. This change was intended to reduce unnecessary treatment of benign or indolent cystic renal masses while preserving a structured approach to lesions that warrant closer surveillance or urologic consultation.[1][2]
For radiologists, the practical importance of the update is that renal mass characterization now relies on more explicit thresholds for septa number, wall or septal thickness, irregularity, and nodules. The Bosniak 2019 MRI update also acknowledges that MRI can detect enhancement and internal complexity not always apparent on CT, which can affect category assignment in selected lesions.[1][3]
What qualifies as a cystic renal mass in Bosniak classification 2019?
Before category assignment, the lesion should first meet the definition of a cystic renal mass. In version 2019, a mass is considered cystic when there is less than approximately 25% enhancing tissue by subjective visual inspection. This distinction is important because predominantly solid masses with necrosis are not intended for Bosniak stratification and should instead be approached within the broader framework of solid renal mass evaluation.[1]
Lesions generally excluded from Bosniak categorization
The Bosniak framework is not intended for every cystic-appearing renal lesion. Important exclusions include lesions with a clear infectious, inflammatory, or vascular explanation, masses with 25% or more enhancing tissue, and lesions arising in hereditary renal tumor syndromes where morphology may underestimate underlying malignant potential.[1]
Technical requirements for accurate Bosniak classification
Reliable application of the Bosniak system depends on appropriate acquisition technique. For CT, evaluation typically requires a renal mass protocol that includes noncontrast imaging and postcontrast imaging, with nephrographic phase images commonly used for enhancement assessment. Thin-section reconstructions help reduce volume averaging and improve evaluation of thin septa, subtle wall thickening, and small enhancing nodules.[1][3]
For MRI, essential components include T1-weighted and T2-weighted sequences, fat-suppressed precontrast and postcontrast T1-weighted imaging, and dynamic gadolinium-enhanced sequences. Subtraction imaging is particularly important for lesions that are intrinsically T1 hyperintense because hemorrhagic or proteinaceous material can mask true enhancement on standard postcontrast images. In those settings, subtraction imaging helps separate native T1 signal from genuine vascular enhancement.[1][3]
Measurement principles
Wall, septal, or nodular measurements should be made on contrast-enhanced images rather than T2-weighted images. Measuring on T2-weighted images can overestimate thickness because debris, hemorrhage, or partial-volume effects may exaggerate apparent wall or septal size. This point is especially relevant when distinguishing minimally thickened structures from thick or irregular enhancing components.[1][3]
Enhancement, septa, wall thickening, and nodules
A central feature of the Bosniak 2019 system is standardized terminology. Enhancement may be defined quantitatively or visually. At CT, measurable enhancement is generally an increase of at least 20 Hounsfield units. At MRI, measurable enhancement is generally a 15% or greater increase in signal intensity on T1-weighted images. Unequivocal visual enhancement also qualifies as enhancement, even when a structure is too small for reliable numeric measurement.[1][3]
Standardized morphologic definitions
Version 2019 provides explicit size-based and shape-based definitions for common descriptors used in complex renal cyst imaging. Septa are described as few when there are 1 to 3 and many when there are 4 or more. Thickness is categorized as thin when 2 mm or less, minimally thickened when 3 mm, and thick when 4 mm or more. An enhancing convex protrusion with obtuse margins that measures 3 mm or less is termed an irregularity, whereas an enhancing convex protrusion with acute margins at any size, or with obtuse margins measuring 4 mm or more, is categorized as a nodule.[1]
These definitions matter because the Bosniak category is driven less by vague overall complexity and more by whether a lesion contains specific findings such as enhancing septations, minimally thickened smooth walls, thick enhancing septa, or definite enhancing nodules. When a lesion satisfies features from more than one class, the highest applicable Bosniak category should be assigned.[1]
| Category | Typical imaging features | Clinical implication |
|---|---|---|
| Bosniak I | Well-defined thin smooth wall, simple fluid, no septa or only imperceptible wall findings. The wall may enhance. | Benign appearance. No routine follow-up is typically required. |
| Bosniak II | Includes lesions with a few thin enhancing septa, homogeneous hyperattenuating nonenhancing masses on CT, homogeneous masses in specified benign attenuation ranges, or homogeneous markedly T2 hyperintense or markedly T1 hyperintense lesions on MRI. | Benign cystic mass. No routine follow-up is typically required. |
| Bosniak IIF | Smooth minimally thickened enhancing wall or septa, or many thin enhancing septa. Also includes certain MRI lesions that are heterogeneously hyperintense on fat-suppressed T1-weighted imaging without visible enhancement. | Usually managed with imaging surveillance because progression, if it occurs, is often detected over time. |
| Bosniak III | One or more enhancing thick walls or septa, or enhancing irregularity of a wall or septum. | Indeterminate lesion with meaningful malignancy risk. Urologic consultation is generally appropriate. |
| Bosniak IV | One or more enhancing nodules, including acute-margin nodules of any size or obtuse-margin nodules measuring 4 mm or more. | Higher likelihood of malignancy. Urologic management discussion is generally warranted. |
How MRI differs from CT in Bosniak 2019
The incorporation of MRI is one of the most important changes in the Bosniak classification 2019. MRI can reveal additional septa, wall irregularity, or subtle enhancement that may not be confidently visible at CT. This can sometimes lead to higher category assignment, especially when thin septa or nodularity become more conspicuous on contrast-enhanced MRI or subtraction imaging.[1][3]
At the same time, MRI also contains class-specific benign patterns not emphasized in CT classification, including markedly T2 hyperintense masses and markedly T1 hyperintense lesions without suspicious enhancement. Accordingly, MRI findings should not be treated as a direct one-to-one translation of CT findings. Instead, MRI has its own strengths in lesion characterization, particularly for hemorrhagic masses, calcified lesions obscuring enhancement at CT, and lesions that remain indeterminate after renal protocol CT.[1][3]
Key changes from Bosniak 2005 to Bosniak classification 2019
The 2019 revision introduced formal definitions for wall thickness, septal thickness, irregularity, and nodularity, and it recognized MRI as a full participant in the classification system rather than a secondary adjunct. Another major conceptual change was rebalancing the system toward specificity. In practice, some lesions previously categorized as Bosniak III under older interpretations may now fall into Bosniak IIF because version 2019 more clearly separates minimally thickened smooth enhancing tissue from thick or irregular enhancing tissue.[1][2]
Comparative studies have shown that version 2019 tends to produce lower sensitivity but higher specificity than version 2005 for malignancy prediction, reflecting its goal of reducing overtreatment of benign lesions. One CT and MRI study also found substantial intermodality agreement between CT and MRI when using version 2019 criteria.[2]
Clinical implications, management language, and reporting strategy
Structured reporting can improve clarity when communicating Bosniak findings. Useful elements include lesion side and pole, maximal diameter, modality used for classification, relevant morphologic features such as septa number and wall thickness, whether enhancement is visual or quantitative, the assigned category, and a concise management-oriented impression. This approach keeps the report focused on the imaging basis for category assignment rather than only listing a final class.[1][3]
Suggested reporting elements
In practice, reports often describe lesion location, maximal size, Bosniak category, and a category-aligned recommendation. Bosniak I and II lesions are commonly described as benign or likely benign with no routine follow-up. Bosniak IIF lesions are typically recommended for surveillance. Bosniak III and IV lesions generally warrant urologic consultation, with subsequent decisions influenced by patient age, comorbidities, surgical candidacy, growth, and institutional management preferences.[1][3]
When MRI is especially useful after CT
MRI is particularly useful when calcifications limit CT assessment of enhancement, when a homogeneous hyperattenuating mass is large, and when a heterogeneous lesion appears nonenhancing at CT but remains indeterminate. In these scenarios, MRI may better define internal architecture, confirm or exclude enhancement, and improve confidence in whether the lesion should remain in a benign-leaning category or move into surveillance or urologic consultation categories.[1][3]
For readers using a Bosniak renal cyst calculator, the most practical lesson is that category assignment should follow imaging definitions exactly. A tool can help summarize the logic of the Bosniak categories, but it should function as a structured aid rather than as a substitute for image interpretation, protocol quality review, or clinical context.
Frequently Asked Questions (FAQs)
What changed in the Bosniak classification 2019 compared with older versions?
The 2019 revision formally incorporated MRI, created precise definitions for septa number, wall and septal thickness, irregularity, and nodularity, and emphasized greater specificity. One effect of this change is that some lesions previously treated as more suspicious under older frameworks may now be categorized as Bosniak IIF rather than Bosniak III when they show only smooth minimal thickening.[1][2]
How is enhancement defined on CT versus MRI for renal cyst classification?
At CT, measurable enhancement is generally defined as an increase of at least 20 HU. At MRI, measurable enhancement is generally defined as a 15% or greater increase in T1-weighted signal intensity. Unequivocal visual enhancement also counts, even if the structure is too small for reliable numeric measurement.[1]
What is the difference between Bosniak IIF and Bosniak III?
Bosniak IIF usually includes lesions with smooth minimally thickened enhancing wall or septa measuring 3 mm, or many thin enhancing septa. Bosniak III requires thicker enhancing tissue of at least 4 mm or enhancing irregularity. The distinction is important because Bosniak IIF is usually managed with surveillance, whereas Bosniak III commonly prompts urologic consultation.[1][3]
When should MRI be preferred over CT for cystic renal lesion evaluation?
MRI is especially helpful when calcification obscures enhancement at CT, when a large homogeneous hyperattenuating lesion remains indeterminate, or when a heterogeneous lesion appears nonenhancing at CT but still raises concern. MRI can also be valuable for hemorrhagic lesions because subtraction imaging improves detection of true enhancement.[1][3]
Can a Bosniak renal cyst calculator replace radiologist interpretation?
No. A calculator may help organize imaging findings and apply category logic consistently, but final classification still depends on image quality, lesion morphology, enhancement assessment, and clinical context. Interpretation of complex cystic masses remains a radiologist task grounded in the Bosniak imaging criteria.
References
- Silverman SG, Pedrosa I, Ellis JH, et al. Bosniak Classification of Cystic Renal Masses, Version 2019: An Update Proposal and Needs Assessment. Radiology. 2019;292(2):475-488. https://pubs.rsna.org/doi/abs/10.1148/radiol.2019182646
- Park MY, Park KJ, Kim MH, Kim JK. Bosniak Classification of Cystic Renal Masses Version 2019: Comparison With Version 2005 for Class Distribution, Diagnostic Performance, and Interreader Agreement Using CT and MRI. AJR Am J Roentgenol. 2021;217(6):1367-1376. https://ajronline.org/doi/10.2214/AJR.21.25796
- Schieda N, Davenport MS, Krishna S, et al. Bosniak Classification of Cystic Renal Masses, Version 2019: A Pictorial Guide to Clinical Use. RadioGraphics. 2021;41(3):814-828. https://pubs.rsna.org/doi/abs/10.1148/rg.2021200160