Acute Cholecystitis Calculator Based on Ultrasound and Clinical Parameters
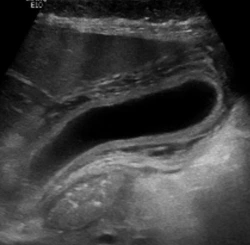
Acute Cholecystitis Calculator Based on Ultrasound and Clinical Parameters
This acute cholecystitis calculator is based on a data-derived risk stratification approach that combines gallbladder ultrasound findings with selected clinical parameters to estimate the probability of acute cholecystitis.[1] It reflects a structured method designed to improve consistency in gallbladder ultrasound interpretation, particularly in cases that do not clearly meet classic diagnostic criteria.
Patel and colleagues describe a framework that addresses a common limitation in radiology reporting. Many gallbladder ultrasound examinations fall into an intermediate category where findings are not definitively positive or negative. This can lead to variability in wording and downstream management recommendations. The proposed model organizes these findings into defined probability categories to support more consistent communication.[1]
The acute cholecystitis risk algorithm proposed by Patel et al [1] synthesizes eleven inputs. Four are non-imaging parameters including age, sex, leukocytosis, and the sonographic Murphy sign. Five are ultrasound-based parameters that characterize gallbladder appearance: gallbladder distention, gallbladder wall assessment, gallbladder contents, presence of a pericholecystic irregular collection, and hepatic artery peak systolic velocity. Two additional inputs allow incorporation of an alternative explanation for symptoms or other imaging findings that substantially increase concern.[1]
A notable feature of this approach is its handling of uncertainty. The sonographic Murphy sign can be positive, negative, or indeterminate. Gallbladder wall thickening is interpreted in context, including distention and possible systemic causes. The model also distinguishes typical sludge from atypical sludge and separates simple pericholecystic fluid from irregular collections that may indicate inflammation. These distinctions align with real-world ultrasound interpretation rather than forcing binary decisions.[1]
Risk Stratification Using Ultrasound and Clinical Parameters
The algorithm progresses in stages. Initial imaging features are assessed, followed by adjustment using hepatic artery peak systolic velocity. A separate non-imaging risk estimate is derived from age, sex, WBC count, and the sonographic Murphy sign. These components are then combined into an overall risk category. Additional modifiers, including green flags and red flags, adjust the final probability depending on the pattern of findings.[1]
Green flags include findings such as a nondistended gallbladder, absence of a sonographic Murphy sign, normal wall appearance, or low hepatic artery velocity. Red flags include definite wall thickening, pericholecystic irregular collections, and other imaging features that increase suspicion. These modifiers allow the model to better reflect clinical nuance rather than relying on a fixed score.[1]
The final output categorizes patients into four probability groups: practically excluded, reduced, elevated, or substantially elevated risk of acute cholecystitis. The substantially elevated group can be further stratified into approximate probability bands of 50%, 75%, and 90% depending on additional modifiers. In the study cohort, observed rates of acute cholecystitis were 0.2% for practically excluded, 8.2% for reduced, 28.2% for elevated, and 60.0% overall for substantially elevated groups, with higher subgroups reaching approximately 90.9%.[1]
This framework is best interpreted as a structured reporting aid for gallbladder ultrasound rather than a replacement for clinical judgment. It provides a consistent way to express probability using ultrasound and clinical parameters, which may help reduce ambiguity in communication between radiologists and referring clinicians.[1] Established guidance such as the Tokyo Guidelines and World Society of Emergency Surgery recommendations similarly emphasize integrating imaging with clinical and laboratory findings.[2][3]
Key points from the acute cholecystitis risk algorithm
| Component | What it includes | Why it matters |
|---|---|---|
| Clinical parameters | Age, sex, WBC count, sonographic Murphy sign | Provides baseline probability context for acute cholecystitis[1] |
| Ultrasound findings | Distention, wall, contents, pericholecystic collection, hepatic artery PSV | Defines imaging-based risk assessment[1] |
| Risk modifiers | Green flags and red flags | Refines probability based on combinations of findings[1] |
| Final output | Practically excluded, reduced, elevated, substantially elevated | Supports consistent probability-based reporting[1] |
Frequently Asked Questions (FAQs)
What does this acute cholecystitis calculator estimate?
It estimates a probability category for acute cholecystitis by combining ultrasound findings and clinical parameters, including gallbladder morphology, sonographic Murphy sign, and laboratory data.[1]
How is acute cholecystitis risk assessed on ultrasound?
Risk is based on a combination of findings such as gallbladder distention, wall thickening, intraluminal contents, pericholecystic abnormalities, and Doppler parameters like hepatic artery peak systolic velocity, interpreted alongside clinical factors.[1]
What does a reduced or elevated probability mean?
These categories reflect estimated likelihood ranges rather than definitive diagnoses. For example, reduced probability corresponds to a low observed rate in the study cohort, while elevated and substantially elevated categories indicate progressively higher observed rates.[1]
References
- Patel MD, Young SW, Patel AG, Chen L, Dahiya N. Evaluating and communicating probability of acute cholecystitis consistently using a data-derived risk stratification algorithm synthesizing ultrasound and clinical parameters. Abdom Radiol (NY). 2026;51(4):1938-1950. doi:10.1007/s00261-025-05203-4. View source
- Yokoe M, Hata J, Takada T, et al. Tokyo Guidelines 2018: diagnostic criteria and severity grading of acute cholecystitis. J Hepatobiliary Pancreat Sci. 2018;25(1):41-54. doi:10.1002/jhbp.515. View source
- Pisano M, Allievi N, Gurusamy K, et al. 2020 World Society of Emergency Surgery updated guidelines for the diagnosis and treatment of acute calculus cholecystitis. World J Emerg Surg. 2020;15(1):61. doi:10.1186/s13017-020-00336-x. View source
The official calculator developed by the authors of Patel et al. paper can be found here.





Well done Dr. Khalighinejad.! Hopefully many users will find this resource valuable.